Hematology in Turkey : Everything you need to know for world-class care
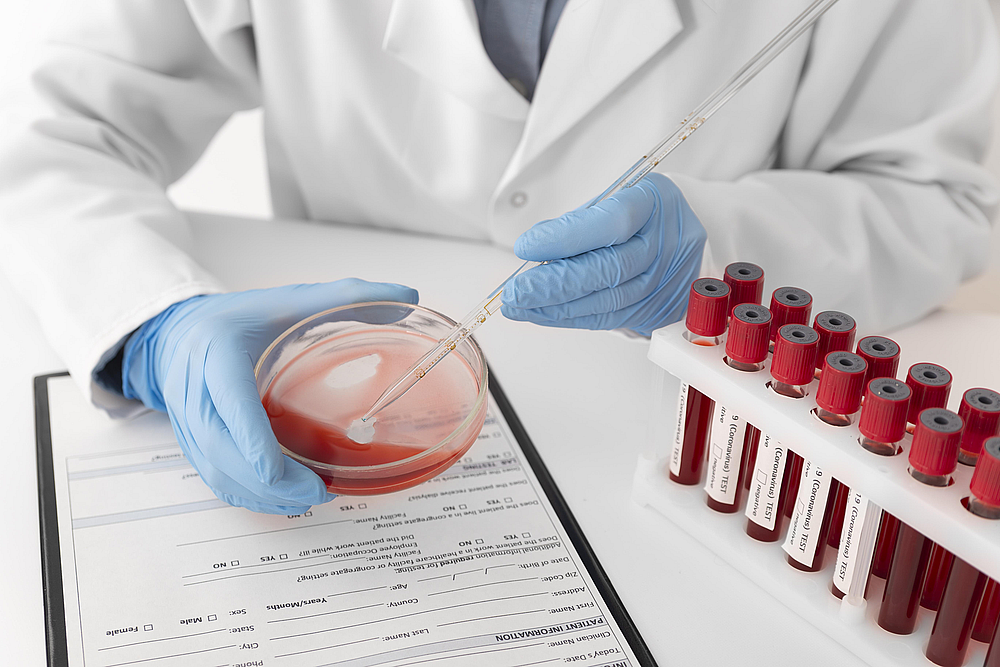
Hematology,the branch of medicine focused on the study, diagnosis, and treatment of blood and hematopoietic system disorders, is now among the most advanced and specialized areas of modern healthcare.
From common conditions such as anemia and clotting disorders to complex conditions like leukemia and lymphoma, effective treatment in hematology requires a precise combination of advanced technology, clinical expertise, and individualized patient management.
As access to specialized hematology services continues to expand globally, more patients are seeking treatment options that combine high standards of medical excellence with affordability and patient-centered care.
Turkey has emerged as a leading destination for advanced hematology care, with hospitals offering internationally accredited services and state-of-the-art medical facilities.
With a focus on comprehensive diagnostics, evidence-based treatment strategies, and multidisciplinary collaboration, Biruni Hospital provides an integrated and supportive environment for patients managing complex hematologic conditions.
With a focus on comprehensive diagnostics, evidence-based treatment plans, and multidisciplinary collaboration, Biruni University Hospital provides a reassuring environment for patients navigating the complexities of blood disorders.
What is Hematology?
A hematology procedure refers to any diagnostic or therapeutic process used to evaluate or treat disorders of the blood and blood-forming organs. These procedures are broadly classified into two categories: diagnostic and therapeutic:
Diagnostic Hematology procedures
These are used to identify and monitor blood-related diseases. Common examples include:
- Complete Blood Count (CBC): A routine test that measures the levels and proportions of different blood cells. It helps diagnose anemia, infections, and many other conditions.
- Blood Smear Examination: A microscopic analysis of blood cells to detect abnormalities in shape, size, or number.
- Bone Marrow Aspiration and Biopsy: Indicated when evaluation of hematopoiesis is required, such as in leukemia or aplastic anemia.
- Coagulation Tests (PT, aPTT): Assess the efficiency of the coagulation cascade and are essential for diagnosing bleeding or thrombotic disorders.
- Flow Cytometry and Immunophenotyping: Advanced tests used to identify types of leukemia or lymphoma by analyzing cell surface markers.
- Genetic Testing and Molecular Diagnostics: Help in identifying inherited blood disorders or genetic mutations associated with blood cancers.
Therapeutic Hematology procedures
These are treatments used to manage or cure blood disorders. They include:
- Blood Transfusion: Replacement of blood or its components (e.g., red cells, platelets) to treat anemia, blood loss, or clotting issues.
- Bone Marrow and Stem Cell Transplantation: Used primarily for blood cancers, where damaged bone marrow is replaced with healthy stem cells.
- Chemotherapy and Immunotherapy: Pharmacologic treatments that target malignant hematologic cells through cytotoxic or immune-mediated mechanisms.
- Iron or Vitamin Supplement Therapy: Prescribed to correct nutritional deficiencies causing anemia.
- Anticoagulation Therapy: Medications like warfarin or heparin used to treat or prevent blood clots.
- Plasmapheresis or Exchange Transfusions: Advanced therapies to remove abnormal components from the blood in conditions like sickle cell disease or autoimmune disorders.
Who needs Hematology Sservices?
You may be referred to a hematologist if you experience symptoms such as:
- Unexplained fatigue or weakness
- Frequent infections or fevers
- Easy bruising or prolonged bleeding
- Pale or yellowish skin
- Swollen lymph nodes or spleen
- Abnormal findings in standard hematologic screening.
These symptoms could point to conditions such as anemia, clotting disorders, platelet abnormalities, blood cancers, or immune-related blood problems.
Benefits of hematology procedures
Early and accurate diagnosis
Hematology tests can identify blood-related issues at very early stages, even before symptoms appear.
This is crucial for conditions like leukemia, lymphoma, and anemia, where early detection significantly improves outcomes.
Individualized treatment plans
Hematologists use detailed blood work and genetic analyses to tailor treatment plans to each patient’s specific condition and biological makeup.
This precision increases the effectiveness of therapy and reduces unnecessary exposure to certain drugs or procedures.
Access to advanced therapies
Patients benefit from access to groundbreaking treatments like:
Bone marrow and stem cell transplantation
Targeted therapies and immunotherapies
Molecular diagnostics for personalized medicine
Risks of Hematology procedures
Although hematology procedures are generally safe and guided by international medical protocols, like all medical interventions, they carry inherent risks similar to other clinical interventions.
These vary depending on the nature of the procedure and the patient’s health condition.
Infection risk
Procedures like bone marrow biopsy or central line placement (for chemotherapy) carry a small risk of infection, especially in immunocompromised patients.
Bone marrow transplant patients may be particularly vulnerable to infections due to suppressed immunity during recovery.
Side effects from Chemotherapy or medications
Chemotherapy drugs used to treat blood cancers can cause nausea, hair loss, fatigue, and increased risk of infection.
Immunotherapy may cause fever, inflammation, or allergic reactions.
Anticoagulants, while preventing dangerous clots, increase the risk of bleeding complications.
Graft-Versus-Host Disease (GVHD)
This is a potential complication after an allogeneic stem cell or bone marrow transplant, where the donor’s immune cells attack the patient’s tissues. It can range from mild to life-threatening.
What are the types of Hematology procedures?
Complete Blood Count (CBC)
A Complete Blood Count (CBC) is a fundamental diagnostic test that evaluates the overall health of an individual by measuring various components of the blood. It provides critical information about red blood cells, white blood cells, hemoglobin, hematocrit, and platelets.
This test is instrumental in detecting a wide range of disorders, including anemia, infections, and hematologic malignancies.
Procedure Steps
- Sample Collection: A healthcare professional draws a blood sample, typically from a vein in the arm.
- Laboratory Analysis: The sample is analyzed using automated machines that count and evaluate the different blood cells.
- Result Interpretation: A physician reviews the results to assess the patient's health status and determine if further testing is necessary.
Bone Marrow aspiration and Biopsy
Bone marrow aspiration and biopsy are procedures used to examine the marrow, the soft tissue inside bones where blood cells are produced.
These tests are crucial for diagnosing various blood disorders, including leukemia, lymphoma, and multiple myeloma.
Procedure steps
- Preparation: The patient is positioned in lateral decubitus or prone position. The biopsy site (usually the pelvic bone) is cleaned and numbed with a local anesthetic.
- Aspiration: A needle is inserted into the bone to withdraw a small amount of liquid marrow.
- Biopsy: A second needle may be used to remove a small core of bone marrow tissue.
- Post-Procedure Care: The site is bandaged, and the patient is monitored for any complications.
Blood transfusion
A blood transfusion involves transferring blood or blood components from a donor to a recipient. It's commonly used to replace lost components due to surgery, injury, or disease.
Procedure steps
- Blood Typing and Crossmatching: Ensures compatibility between donor and recipient blood.
- Preparation: The patient is prepared, and vital signs are monitored.
- Transfusion: Blood is transfused intravenously over a set period.
- Monitoring: The patient is observed for any adverse reactions during and after the transfusion.
Coagulation tests (PT, aPTT, INR)
Coagulation tests assess the blood's ability to clot and are essential for diagnosing bleeding disorders or monitoring anticoagulant therapy.
Procedure steps
- Sample Collection: Blood is drawn into a tube containing anticoagulant.
- Laboratory Analysis: Tests like Prothrombin Time (PT),Activated Partial Thromboplastin Time (aPTT),and International Normalized Ratio (INR) are performed.
- Result Interpretation: Results help determine clotting efficiency and guide treatment decisions.
Hemoglobin electrophoresis
Hemoglobin electrophoresis is a test that identifies different types of hemoglobin in the blood, aiding in diagnosing disorders like sickle cell anemia and thalassemia.
Procedure steps
- Sample Collection: Blood is drawn and prepared for analysis.
- Electrophoresis: The sample is placed in a gel, and an electric current separates the hemoglobin types based on their charge.
- Analysis: The separated hemoglobin bands are analyzed to identify abnormalities.
Bone Marrow transplantation
Bone marrow transplantation involves replacing damaged or diseased bone marrow with healthy stem cells. It's used to treat conditions like leukemia, lymphoma, and severe anemia.
Procedure Steps
- Pre-Transplant Conditioning: Patients undergo chemotherapy or radiation to destroy diseased marrow.
- Stem Cell Collection: Healthy stem cells are collected from a donor or the patient.
- Transplantation: The stem cells are infused into the patient's bloodstream.
- Engraftment and Recovery: The new stem cells migrate to the bone marrow and begin producing healthy blood cells.
Flow cytometry
Flow cytometry is a laboratory technique used to detect and measure physical and chemical characteristics of a population of cells or particles. It's commonly used in diagnosing blood cancers.
Procedure Steps
- Sample Preparation: Cells are suspended in a fluid and treated with fluorescent markers.
- Analysis: The sample passes through a laser beam in the flow cytometer, and detectors measure the light emitted.
- Data Interpretation: The information gathered helps identify specific cell types and abnormalities.
Peripheral Blood smear
A peripheral blood smear involves spreading a drop of blood thinly onto a microscope slide, staining it, and examining it under a microscope. It helps in diagnosing various blood disorders.
Procedure Steps
- Sample Collection: A blood sample is obtained via finger prick or venipuncture.
- Slide Preparation: A drop of blood is placed on a slide and spread to create a thin film.
- Staining: The slide is stained to differentiate blood cell types.
- Microscopic Examination: A specialist examines the slide for abnormalities in blood cells.
What are the necessary preparations before undergoing a Hematology procedures?
Personal preparations
These are the steps you should take on your own or with the help of your caregiver or support system. They focus on physical, emotional, and lifestyle readiness to ensure the procedure goes smoothly.
Maintain a Balanced Diet
In the days leading up to your procedure, eat a nutrient-rich diet. Iron, folate, vitamin B12, and protein are particularly important for blood health. Avoid processed foods and excessive sugar.
Stay Hydrated
Proper hydration helps your veins become more accessible for blood draws and IVs. Aim to drink at least 1.5 to 2 liters of water daily unless advised otherwise.
Avoid Alcohol and Tobacco
Alcohol can interfere with your blood chemistry, and smoking affects circulation and immune function. Refrain from consumption at least 48–72 hours prior to the procedure, unless otherwise directed by your physician.
Limit Physical Strain
Avoid heavy physical activity the day before the procedure, especially if you're undergoing something invasive like a biopsy or bone marrow aspiration.
Get Adequate Sleep
Ensure you are well rested. A minimum of 7–9 hours of sleep the night before helps the body regulate stress hormones and maintain healthy blood pressure.
Communicate Any Symptoms
If you feel unwell, have a fever, or experience unusual symptoms such as fatigue, bruising, or dizziness, inform your healthcare team as it might affect your test results or safety.
Fasting if Required
Some hematological tests or pre-treatment screenings may require fasting. Always ask if you need to avoid food or drink beforehand, and follow instructions closely.
Emotional Readiness
Stress can impact blood pressure and immune response. Engage in light breathing exercises or meditation to help stay calm. Knowing what to expect can reduce anxiety.
Wear Comfortable Clothing
Loose clothing makes it easier for blood draws, IV insertion, and physical examinations. For procedures involving the bone marrow, ensure the biopsy site is easily accessible.
Arrange Transportation
Some procedures might leave you feeling weak or drowsy. Arrange for someone to drive you home or accompany you if sedation or pain management is involved.
Preparations With the Doctor
These steps are essential for both safety and procedural accuracy. They involve communication, diagnostics, and medical planning with your hematologist or care team.
Full Medical History Review
Provide a complete history of previous illnesses, chronic conditions, surgeries, medications, allergies, and family history of hematologic disorders. This helps identify risks and guide procedure choices.
Medication Management
Certain medications can affect blood clotting, immune response, or interact with anesthesia. Your doctor might instruct you to stop or adjust these medications prior to the procedure, especially anticoagulants, antiplatelets, or NSAIDs.
Pre-Procedural Blood Tests
Often, initial tests such as a basic CBC, clotting profile, or metabolic panel are required to assess your baseline condition. These ensure you're fit for further hematologic investigation or treatment.
Imaging Studies if Necessary
Some procedures, like biopsies, might require pre-imaging (e.g., ultrasound or CT scan) to identify the most suitable site for sampling and minimize complications.
Consent and Explanation
Your doctor will review the nature of the procedure, its purpose, potential risks, and expected outcomes. You’ll be asked to sign a consent form, which is also your opportunity to ask questions.
Allergy and Sensitivity Screening
Your team may perform skin tests or review records to ensure you don’t have allergic reactions to anesthesia, antiseptics, latex, or contrast agents, depending on the procedure.
Infection Control Measures
If you're immunocompromised or scheduled for a transplant, you'll be screened for infections and may receive antibiotics or antivirals as precautionary measures.
Vaccination Review
For procedures like bone marrow transplants, your doctor might check your vaccination status and recommend certain vaccines to protect you during immunosuppressive treatments.
Nutritional and Supplement Guidelines
Your hematologist may refer you to a dietitian or provide guidelines regarding supplements such as iron, B12, or folic acid, particularly if you're being treated for anemia or a deficiency.
Hospital Admission Preparation
For more invasive or long-duration procedures, you'll be guided through hospital admission steps, including what to bring, how to prepare your home for return, and post-procedural care planning.
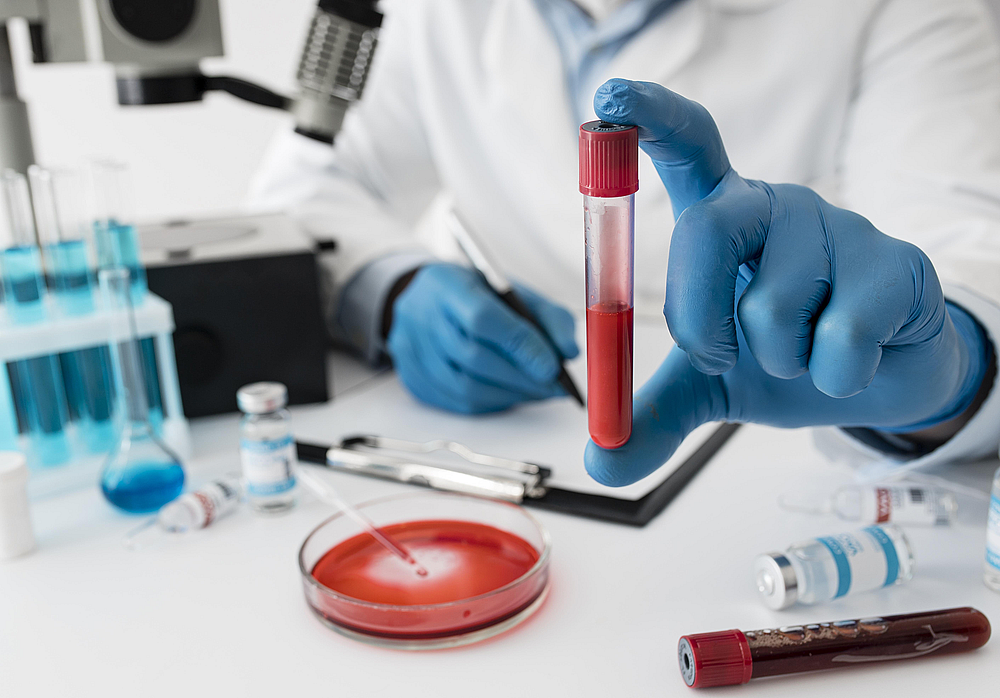
What Happens During a Hematology Procedure?
Patient Positioning and Site Preparation
Once the procedure begins, the patient is guided to sit or lie down in a specific position based on the type of hematology procedure being performed. The chosen body part (arm, hip, chest, etc.) is then prepared for entry.
Doctor’s Actions:
- Guides the patient into the correct posture for accessibility and safety
- Identifies the correct vein or bone site using palpation or visual aids
- Cleans the selected area using antiseptic solution to prevent infection
- Drapes sterile cloths around the area to maintain a sterile field
Local Anesthesia Application (if required)
For procedures such as bone marrow biopsy, the area is numbed to minimize pain. Even minor procedures may involve a mild anesthetic to reduce discomfort.
Doctor’s Actions:
- Draws up a local anesthetic (usually lidocaine) into a syringe
- Inserts the needle just under the skin and into deeper tissue
- Monitors the patient for any allergic reaction or discomfort
- Waits a few minutes to allow the anesthesia to take effect
Insertion of Needle or Cannula
Depending on the procedure, a fine needle or intravenous cannula is inserted into the appropriate vein or bone.
This is the access point for drawing samples, administering substances, or collecting marrow.
Doctor’s Actions:
- Chooses the correct needle gauge based on procedure type
- Inserts the needle at a precise angle, slowly and carefully
- Confirms correct placement via blood flow or physical feedback
- Stabilizes the needle or cannula using tape or a securing method
Sample Extraction or Fluid Administration
This is the core action of many hematology procedures—either removing fluid for diagnosis or introducing blood components for treatment.
Doctor’s Actions:
- Draws out blood or bone marrow into specialized tubes
- Collects multiple vials if different types of analysis are needed
- Ensures the sample is sufficient and uncontaminated
- In transfusions, connects IV tubing to start the blood flow
Monitoring of Patient Response
Throughout the procedure, the doctor closely observes how the patient’s body is responding, looking for early signs of complications such as allergic reactions, faintness, or bleeding.
Doctor’s Actions:
- Monitors vital signs (heart rate, blood pressure, oxygen levels)
- Engages in light conversation to assess patient alertness
- Watches for skin changes, respiratory difficulty, or discomfort
- Adjusts or pauses the procedure if needed
Stepwise Advancement or Retraction (for bone procedures)
For procedures like bone marrow biopsy or aspiration, the needle is carefully advanced through soft tissue and bone, then withdrawn in specific stages to maximize quality of the sample.
Doctor’s Actions:
- Uses a twisting or pushing motion to access the bone
- Applies steady pressure to avoid cracking or damaging the bone
- Once the needle is in the marrow space, uses a syringe to aspirate
- For biopsy, removes a core sample using a trephine needle
Sample Handling and Labeling
Collected specimens are handled with extreme care to maintain accuracy. Each tube or slide is immediately labeled and secured to avoid cross-contamination or identification errors.
Doctor’s Actions:
- Transfers fluids or marrow onto prepared slides or into containers
- Labels each sample clearly with the patient’s identification
- Applies preservative or anticoagulant if needed
- Hands off the samples to lab personnel or places them in secure storage
Hemostasis (Stopping the Bleeding)
After the sample or treatment is complete, the doctor ensures that bleeding is completely stopped using pressure and specialized materials.
Doctor’s Actions:
- Applies gauze and firm pressure to the puncture site
- If bleeding continues, uses hemostatic agents or clotting patches
- Examines the site for swelling, discoloration, or active bleeding
- Applies sterile bandages once bleeding has stopped
Observation Window (in transfusions or invasive procedures)
In more complex procedures like transfusions or aspirations, a brief observation period is often included mid-way to ensure continued safety before proceeding further.
Doctor’s Actions:
- Performs interim assessment of patient comfort and stability.
- Asks questions about dizziness, chest pain, or nausea
- If any issue arises, administers medication or halts the procedure
- Continues only if the patient is stable and responsive
Safe Needle or Instrument Removal
The final step involves the careful removal of any instruments or needles, ensuring no damage to the surrounding tissues and reducing the risk of infection or bruising.
Doctor’s Actions:
- Gently pulls out the needle at the same angle it was inserted
- Ensures no remnants or fragments are left inside the tissue
- Applies a clean dressing to prevent infection
- Provides initial wound care if necessary
The post-operative period after the hematology procedure
Post-procedural recovery is a critical component of hematologic care. Whether it’s a diagnostic test like a bone marrow biopsy or a treatment like a transfusion, what happens afterward affects how well your body heals and responds.
Recovery is typically divided into two phases: the short-term recovery period, which covers the first few days, and the long-term recovery period, which can last several weeks or even months depending on the type of procedure.
Short-Term Recovery (First Few Days)
This phase is about immediate care, rest, and early monitoring.
Monitoring Vital Signs
Right after the procedure, healthcare staff will monitor your heart rate, blood pressure, and how you're feeling. This helps detect any early complications, such as allergic reactions or bleeding.
Pain and Discomfort Management
You may feel soreness or discomfort, especially after procedures like marrow biopsies. Doctors usually prescribe mild pain relievers, and cold packs may help with swelling.
Wound Care
If you have a biopsy or any invasive procedure, the area will be cleaned and bandaged. You’ll receive instructions on how to keep it clean and when to change the dressing.
Activity Limitations
For the first 24 to 72 hours, it's important to rest. Avoid heavy lifting, bending, or any physical strain.
Light Eating and Hydration
Stick to simple, easy-to-digest foods at first. Drinking plenty of water helps your body recover, especially if blood was taken or if you received sedation.
Medications
You might be given antibiotics to prevent infection, anti-inflammatories for swelling, or supplements to support your blood health.
Emotional Wellbeing
It’s common to feel tired or emotionally drained. Don’t hesitate to talk about it—your healthcare team is there to support you.
Signs to Watch For
Patients should contact their healthcare provider if they experience fever, persistent bleeding, or severe pain.
Return to Normal Activities
Most people can return to daily tasks after a couple of days, though full recovery depends on the specific procedure.
Follow-Up Appointments
Your doctor will schedule check-ins to go over your results and decide if more treatment is needed.
Long-Term Recovery (Weeks to Months)
Once the initial healing phase is over, your body continues to repair and stabilize.
Blood Cell Regeneration
If the procedure involves marrow or cell sampling, your body will slowly replenish blood cells. This process takes time and energy.
Immune System Recovery
Depending on your procedure, your immune system may need time to return to full strength. You may need to avoid crowds or sick individuals during this phase.
Ongoing Symptoms
Fatigue, mild pain, or weakness can linger. These usually fade with rest and good nutrition.
Long-Term Medications
You may continue medications for several weeks or longer to help your recovery or manage any blood conditions.
Lifestyle Adjustments
Healthy habits, like eating iron-rich foods, staying hydrated, and avoiding smoking—support your recovery and overall blood health.
Physical Activity
Gentle movements and walking can help circulation and prevent stiffness. Avoid intense exercise until cleared by your doctor.
Emotional Recovery
Some people experience anxiety, especially if their procedure is part of a larger treatment journey. Support is available if you need it.
Nutrition Support
A balanced diet rich in protein, iron, and vitamins is key to healing. You might meet with a nutritionist if needed.
Regular Checkups
You’ll have routine blood tests and exams to track your progress and catch any delayed complications.
Full Return to Normal Life
For many, recovery leads back to a regular routine. For others, especially those undergoing long-term treatments, recovery is ongoing but manageable with care and support.
Conclusion
Turkey has established itself as a reputable destination for advanced hematology treatments,at affordable prices.
Combining medical expertise, cutting-edge technology, and patient-centered care services, Turkey continues to attract individuals worldwide in their quest for quality healthcare.



